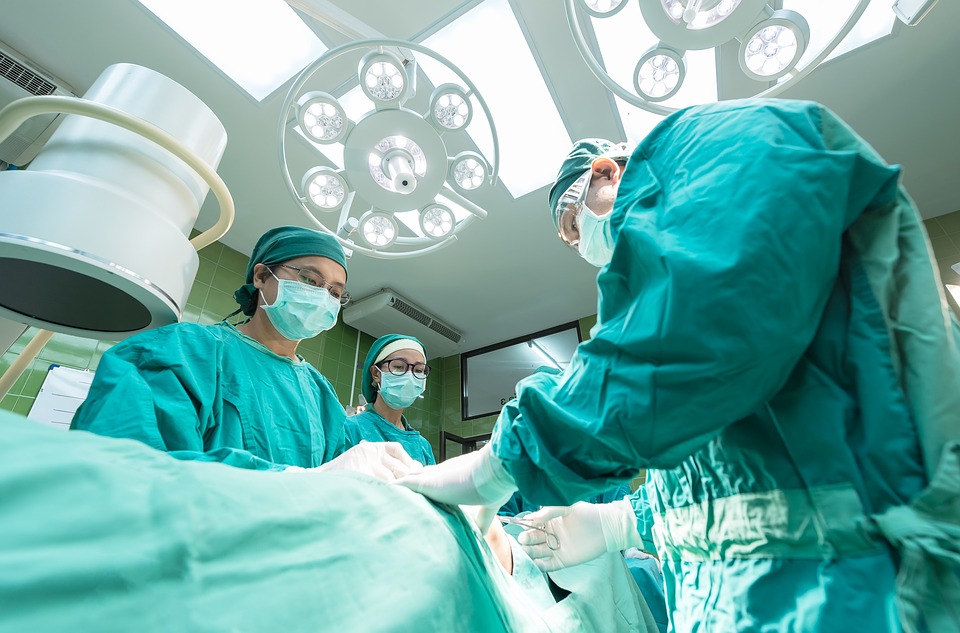
The Care Quality Commission (CQC) has found that two-fifths of private hospitals in the UK are not meeting basic patient safety standards. So what does this mean for patient care, and can private hospitals be held accountable using human rights?
In the first comprehensive inspection of independent acute hospitals in England, 206 hospitals were inspected, with 30 percent given an overall rating of ‘requires improvement’. The main areas of concern were safety and leadership.
‘Risks in Operating Theatres Due to Informal Practices’
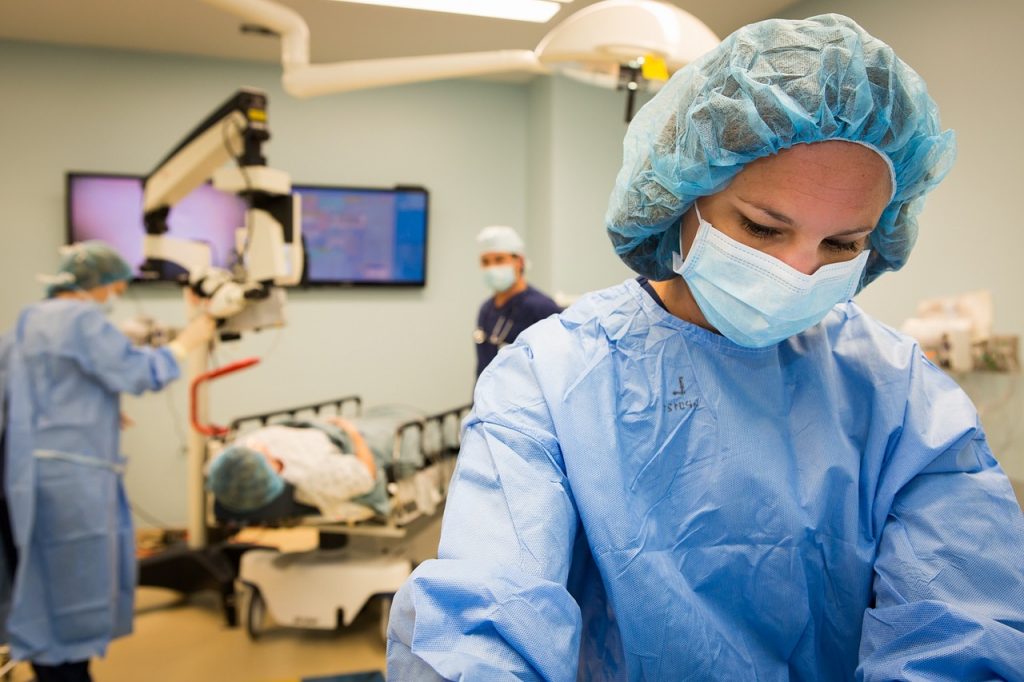
Image Credit: TheShiv76 / Pixabay
There was a “lack of a culture of learning from incidents and a weakness around incident reporting,” according to report. Inspectors also found “risks in operating theatre safety due to informal practices” and even “a few instances where the World Health Organisation surgical checklist was not being followed rigorously”.
The other main concern was a lack of formalised governance procedures. Some hospitals will include consultants who work under “practising privileges”, and the CQC found that there is sometimes a lack of oversight or monitoring of the consultants’ work.
A few instances where the World Health Organisation surgical checklist was not being followed.
CQC Report
These concerns about governance meant that 30% of the hospitals were rated, in terms of leadership, as “requires improvement”, and 3 percent as “inadequate”. The CQC also identified a lack of expertise among some nursing staff, meaning that some nurses lacked the knowledge and skills required to care for all patients on their ward.
However, there were some positive findings in the report. After assessing whether private healthcare services are safe, caring, responsive, effective and well led, the providers were given an overall rating. Inspectors found that most were providing good care, with 70% rated “good” or “outstanding”. The inspected healthcare providers also responded well to the CQC’s recommendations, and they have been quick to address areas of improvement.
What Does This Mean for Patient Rights?
Image Credit: Marcelo Leal / Unsplash
When it comes to private hospitals, it can be tricky to navigate the human rights obligations under the Human Rights Act (1998), as this legislation generally only applies to public authorities. However, private hospitals providing NHS services and performing public functions may come under the scope of the Act, which means they must respect and protect human rights when they provide health and care services.
The CQC report follows a national inquiry into private sector health providers and is the first comprehensive analysis of the quality of care provided by independent acute hospitals. Also, it’s important to note that they apply a human rights approach in their inspection and regulation.
This means they must consider the following human rights principles when assessing standards of care: fairness, respect, equality, dignity, autonomy and right to life. If they find any human rights breaches, they may be able to address these through their own powers. Or alternatively, they may need to refer cases to more suitable regulatory bodies such as the Equality and Human Rights Commission.
We must continue to promote a culture, in all types of healthcare, where patient safety concerns are not brushed aside.
Royal College of Surgeons
The malpractice of surgeon Ian Paterson, for example, who was jailed for 20 years for grievous bodily harm and wounding with intent, resulted in calls for greater regulation of private healthcare. There is a need for proper oversight of doctors and staff operating in private hospitals, especially consultants. The CQC noted that consultants were often treated as ‘customers’ bringing business to the hospital, and that managers can be reluctant to challenge them.
However, as the president of the Royal College of Surgeons stresses: “We must continue to promote a culture, in all types of healthcare, where patient safety concerns are not brushed aside”.