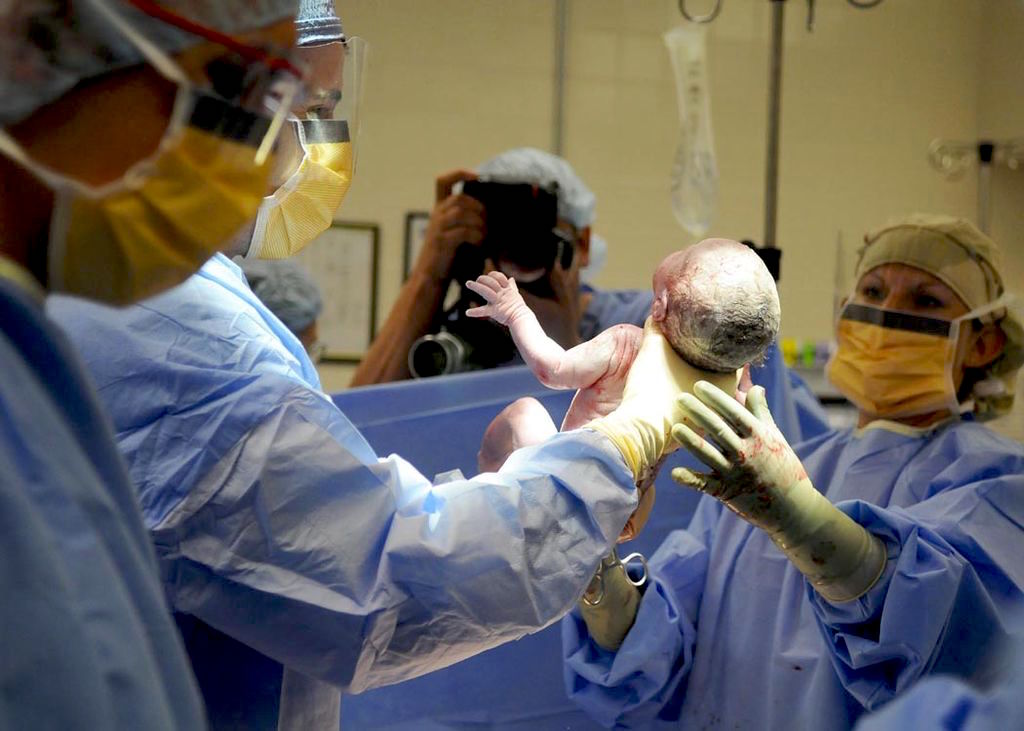
The delivery pager goes off again whilst I’m examining a baby. I apologise to the mum, wash my hands, and quickly call the number listed on my pager. The call is promptly answered by a midwife, “Is that the paediatrics doctor? We need you on the labour ward, room four”.
When I arrive, the midwife updates me on the situation and indicates I need to be there at the delivery in case the baby needs some help adapting to life outside the womb. In this instance, I need to take the baby straight around to the neonatal unit to take some blood tests and administer antibiotics after birth. Evidence has shown us that once certain risk factors are identified, antibiotics should be started within one hour. I hurry round to room four. The obstetrician is assisting the baby’s entrance to the outside world, as the mum’s body isn’t managing on her own. She has lost a lot of blood. The obstetricians can decide if she needs a transfusion soon, but right now, the mum’s main concern is her baby. It’s a boy!
He is transferred straight to my heated table. I dry and wrap him up in warm towels. He cries without any further intervention, and we all smile with relief and joy as we witness this baby’s first breaths. I tell the mum I need to take her boy away briefly, and re-explain the need for antibiotics. She agrees and permits me to take her baby boy to the unit. Making sure patients are informed about their treatment, can make their own decision is a key part of being a good doctor – and a key part of our human rights.
‘Before I can even get started, the delivery bleep goes off again’
 His dad comes with me, grinning ear-to-ear as we push a cot containing his well-wrapped boy to the neonatal unit. Inserting a cannula into his hand, taking blood tests, administering antibiotics and examining him all takes a little while, and we re-unite him with his mum 65 minutes after we took him away. We know that the prognosis is very positive for him as we identified potential problems before they arose. I return to my busy list of outstanding jobs, and before I can even get started, the delivery bleep goes off again…
His dad comes with me, grinning ear-to-ear as we push a cot containing his well-wrapped boy to the neonatal unit. Inserting a cannula into his hand, taking blood tests, administering antibiotics and examining him all takes a little while, and we re-unite him with his mum 65 minutes after we took him away. We know that the prognosis is very positive for him as we identified potential problems before they arose. I return to my busy list of outstanding jobs, and before I can even get started, the delivery bleep goes off again…
A couple of evenings later, I hear from my friend volunteering as a doctor in part of Africa. She shares her frustration with the resources there compared to our NHS. Their neonatal unit only has 5 incubators which is simply not enough, they do not have any ventilators to assist babies with breathing, and most mums do not have screening during pregnancy, so potential problems cannot be prepared for. Blood tests are extremely limited, and sometimes their unit has a power cut.
In the UK, our NHS encourages the right to health: facilities and services are accessible to all, regardless of income or social standing. Patients are treated with dignity and respect, a key part of our human rights. Our system is under a lot of pressure, but should be treasured. The things that we take for granted as due procedures are incomparable to the challenges hospitals face in some parts of the world. Not everyone is so privileged.
Melody Redman is a junior doctor training in clinical and academic paediatrics in Yorkshire. She is a representative of the British Medical Association Junior Doctors Committee.